Value and Opportunities Created by Ontario’s Digital Health Assets
On October 7, 2016, the Minister of Health and Long-Term Care wrote an open letter to Ed Clark in his capacity as the Premier’s Business Advisor and Chair of the Advisory Council on Government Assets to assess the value and opportunities created through the digitalization of Ontario’s health care system. This report is Ed Clark’s response.
Dear Minister Hoskins,
On October 7, 2016, you wrote me asking that I review Ontario’s digital health assets and all related intellectual property and infrastructure, and make recommendations on maximizing the value of these assets for the people of Ontario.
I have approached these questions, as I know you and the government do, from a belief that our public health care system is both an essential fabric of our society, but also a potential differentiator in helping to grow a modern economy. As you are aware, I have spoken passionately on many occasions about the importance of preserving our public health care system, both as a statement of who we are as a people and the values we hold, but also as a foundation for creating, along with our public education system, a society where everyone can reach their full potential. I have therefore approached the questions you have posed from that point of view – have our current digital health assets created value to strengthen our health care system? Has eHealth Ontario – the agency that has built and operated the foundational infrastructure for this system – created value? Could it create more? And what more needs to be done to use our digital health assets to produce better clinical outcomes and improve patient experiences?
I will explain briefly how I tackled these questions, but it is important to first put into context our current digital health care system. eHealth Ontario’s work, while foundational in nature, reflects only a portion of the activities taking place across Ontario’s health care sector to digitalize health care. Work is going on across multiple organizations to bring health care in line with 21st century standards for storing, transferring, making available and using information. We have in the province: 29,000 physicians, 150,000 nurses, thousands of other health care providers, 14 Local Health Integration Networks, 156 hospital corporations that operate 238 hospital locations, 14 Community Care Access Centres, 36 public health units, 76 community health centres, more than 4,000 pharmacies, 23 active community laboratories, and 928 independent health facilities (36 ambulatory and 892 diagnostic). All are creating important health information about Ontario’s 14 million patients and health care service users, and all need information to provide the best care possible for patients.
It quickly became clear to me that valuing our digital health assets and the work of eHealth Ontario, the agency, could only be done in the context of the whole. The mandate of eHealth Ontario was to build the basic infrastructure of the system – the connected backbone – and the data repositories and viewers for the system, to which all else could be attached. Most of the assets that have been created lie outside of the control of eHealth Ontario. So my first conclusion was that we had to look at all of the digital health assets created by the Province of Ontario (Province) including, of course, eHealth Ontario.
The next step was to define value. I will get into this again later, but essentially value could be defined by:
- Producing better clinical outcomes;
- Improving patient experiences;
- Reducing health care system costs;
- Enabling data analysis to improve the quality of health care; and
- Stimulating economic growth.
So what value has been created and what value could be created?
As it happens there is, as you know, a federal agency – Canada Health Infoway (Infoway) – which has been established to both promote and evaluate digital health assets. This agency produces a number of studies and its work is rigorously evaluated. So we have a third party source that estimates value.
Unfortunately, Infoway only looks at some of the programs that are supported to create digital health assets. Examples of assets not captured by Infoway’s estimate of benefits for Ontario include:
- Ontario Laboratory Information System (OLIS);
- Cancer Care Ontario systems;
- Panorama;
- Community Support Services systems;
- Community Care Information Management systems; and
- Community Mental Health and Addictions systems.
The estimates also do not take into account the value of data analysis in improving health care or the economic benefits of digital health expenditures. Finally, it is not possible to put a dollar value on lives saved, or stress reduced for patients. All of our experts supported a view that the Infoway value estimates significantly underestimate the true value of our digital health assets.
With these caveats, what do the Infoway studies tell us? Ignoring the benefits not included, in 2015-16 Ontario’s digital health assets generated annual benefits of $900 million per year. To put this into context, the Ministry of Health and Long-Term Care (Ministry) would estimate that their spending on digital health assets, including on agencies not covered in Infoway’s valuation of benefits, was just under $900 million in 2015-16. If we included all the benefits not counted, the extent to which benefits exceed costs would be quite large. In short, our investments in digital health have brought us to a point where the ongoing value created significantly exceeds the province’s cost to maintain and grow our digital health assets. This is a major milestone.
Equally important, as I worked my way through this file, it became obvious that we have created huge potential value. The analogy I came to use was the building of a highway. In the early years it has only costs, and little value. As ramps and feeder roads are built, the highway has more and more value. In Ontario’s case, there are many ramps and feeder roads that are still to be built. Our experts told us that if we can just build these ramps and feeder roads, the value of our previous investments will increase drastically.
We can use the same Infoway studies to get a sense of a cumulative minimum value over the years. For Ontario, Infoway in their written submission put the value for the period of 2007-2015 at $5.7 billion (in constant 2015 dollars). A big number, but again it is worth noting that it is only a partial estimate – the true valuation would be significantly higher.
So, Minister, you can be assured that significant value has been created, and that the ongoing value well exceeds the costs of maintaining and growing our digital health assets, and Ontario is well positioned to add significant increased value.
Let me take you through how I came to this conclusion and more particularly, how I came to views as to how to realize the full potential of what has been built.
Initially when I accepted this assignment, I wondered how a banker could possibly comment on this topic. Well, at the risk of over analogizing, there are many parallels to running systems for a large bank. TD, at the time I was CEO, had 23 million customers served by 2,400 branches across North America, with customer access provided 24 hours a day, seven days a week, and with security and privacy protections built in. The technical issues of running such a system and running a health care data system are not so different. The people and organizational issues certainly are. In addition, the degree of focus on providing the customer/patient with information is strikingly different.
Notwithstanding the possible similarities, I clearly needed to get up the learning curve quickly. I decided to engage the health care community to the largest extent practical. Recognizing the time constraints of my assignment, I must acknowledge and apologize that there may have been groups or individuals that I did not have an opportunity to hear from. In the end I spoke with more than 30 different expert individuals and groups and asked 33 of them to produce a short submission on how they would describe their perceptions of digital health assets and their associated value. These documents, plus the conversations that I had with experts when soliciting help, were invaluable. I also asked for submissions from the Ministry and from eHealth Ontario. In addition, I received expert input from Brian Beamish (Information and Privacy Commissioner of Ontario), Jennifer Zelmer (President, Azimuth Health Group and previous Executive Vice-President at Canada Health Infoway), Dr. John Halamka (International Health Care Innovation Professor at Harvard Medical School and Chief Information Officer of the Beth Israel Deaconess Medical Center), Dan Sheldon (Digital Strategy Lead for the UK Department of Health), and Graham Scott (Chair of the Board, Canada Health Infoway). I convened a smaller number of the authors, with whom I shared these submissions and discussed key themes and recommendations to the government. Again, these conversations were extremely helpful. Naturally this final document and its recommendations are mine and mine alone.
I think it is important to note that all of those whom I contacted enthusiastically took up the challenge. There is no question that all would say that the digitalization of health care is absolutely essential, and share my emphasis on its role in preserving our public health care system. They generally all agreed that its benefits, which in some ways are hard to calculate, far exceed the costs. And they would also say we have made great progress but can achieve much more, not only with advances in IT, but also by modernizing health care practice patterns, policies, and other elements of our health care system to take full advantage of the opportunities that digital health offers. As to eHealth Ontario the agency, there was a clear view that it is time to move on from focusing on past issues. eHealth Ontario has accomplished a lot. Yes, eHealth Ontario may have stumbled in the past. And yes, it has not always met what were very ambitious timelines. But it has built core infrastructure that is now creating real value for Ontarians. It is in the process of delivering critical additions to that infrastructure. And our experts would agree that the management changes that you, Minister, initiated in 2014, with respect to eHealth Ontario, have made the agency under its current leadership, a much improved organization.
There was some disagreement about the details around what needs to be done and how. But there is a deep consensus that we should not slow the journey, but speed it up, and a deep hope, indeed almost a plea, that we can do so in a factual, non-partisan, non-political way. Health care is too important t not to have all our suuport.
I would add my personal support of these views. Having lived in a fully digitalized world focused on getting customers what they want, when they want, and today spending my time focused on how Ontario can ride the wave of a tremendous base we have in the innovation economy, it does seem strange that probably our most important sector, our health care system, is behind the times. But I have also been struck by how many pieces have already been put in place. Maybe not according to a master plan. This might be disconcerting to some, less so to me. Technology is moving so fast that we don’t necessarily want to lock in one universal same world. Instead we should focus on inter-operability, standardization of protocols, and flexibility to adapt. We must be tough on setting and meeting these standards. We should leave room to tap into the innovation economy and ensure competitiveness, all in a way that upholds patient privacy.
The other comment that I would make concerns the concept of the “last mile”, which one could really argue is the first mile when it comes to providing patients with access to their health records. Because of the approach the Province has followed, which has been quite permissive, we have built many pieces, but the full value of our digital health assets will not be realized unless patients are connected. Here the last mile – that is to say, the ability of health care providers and patients to both access and contribute to digital records – matters enormously. This is really a case where everyone has to contribute if patients are to fully benefit – health care organizations, providers, practitioners, agencies, and government. Today the value of what has been accomplished is less than what it could be because we have not fully developed the last miles. To date, the Province has been very successful in getting community-based physicians and nurse practitioners to install electronic medical record (EMR) systems. Few however, use them to their full potential to support clinical practice (e.g. to proactively identify and reach out to patients who would benefit from preventive or follow-up care) or to share key information needed to improve care coordination (e.g. with specialists or home care nurses). We are on the verge of unleashing significant value if we push on. Getting the last miles built and deepening clinical use must be areas of key focus.
Finally I must comment on the lack of patient orientation. I understand the health care sector’s tendency to focus on the health care practitioner first – the need to ensure that they have as much information as possible so that they can provide the best possible care for patients, and the need to build systems that can be used seamlessly in their workflow to create digital records, including pushing data into the system, and pulling data from the system. I also acknowledge that progress towards focusing on the patients has been made. The government’s health strategy, Patients First: Action Plan for Health Care is patient-focused and the work that the Ministry has undertaken to date in developing a digital health strategy is grounded in putting the needs of Ontario’s patients first. But there is a long way to go to realize the vision the Ministry has laid out in its strategy. Patients not only have a right to know their health information; they can be important contributors. They are verifiers of the facts and manage their health on a daily basis. Increasingly today, patients themselves understand medical issues and can sense if things are wrong. They will be a force of support, and rigid critics of the digital system – wanting up-to-date information and online services in easily accessible forms. So in simple terms we must build a patient-centric information system. If we do that we will build a system that adds value for all stakeholders.
So let me outline how this report is laid out. First, I provide a brief description of the system and its history. Then I deal with the question of value. I also explore the themes that run through the submissions I received, and the discussions I had. There is a fair degree of consensus among experts on these themes. Finally, I lay out my recommendations on how to create more value. In short, we need a more clearly defined digital health strategy and one that links to the overall strategy for health, with more clearly defined roles, and a shift from a permissive to a more directive approach to the adoption of and creation of digital records.
I struggled with how aggressive I should make the targets I propose for implementation of a digital health strategy. I was conscious of the history of setting goals that were subsequently not met. On the other hand, it was clear that the community of leaders in health care were anxious for tough goals. Without tough goals there was a risk that the various actors would not feel the urgency of the need to change. The prize is very large indeed – better outcomes and lower costs. The effort must be both urgent and significant. I opted for tough goals.
As I prepared this report, I was struck by how many previous reports have been written, studies have been conducted, task forces launched, consultant exercises initiated. There has indeed been an enormous amount of work done; undoubtedly necessary not only to help people get to the right conclusion but to form a consensus around those conclusions. I have been the beneficiary of this work, but I would also observe that the time is now for action and we must choose a way forward and make it happen.
In simple terms we have come a long way. We are clearly creating more value than we are spending. Making last mile connections and increasing clinical and patient use of our digital health assets will redefine the value of what we have already done. Much more can be achieved with a more focused, directive approach with tough milestones, close project management, and appropriate enablers of change.
Sincerely,
Ed Clark
Chair of the Advisory Council on Government Assets and Business Advisor to the Premier
Context
Digital innovation
No one would disagree that we live in a time where digital innovation is progressing at a speed like we have never seen before. Banks, commercial retailers, and travel and hospitality providers have been actively adopting and integrating modern technology, security and privacy protections into their online services for the last 20 years – not only to improve and create administrative efficiencies in their own business practices, but to meet customer demand for fast, easy, and convenient online experiences and to enable new customer experiences and products otherwise not possible. Digital innovation has also spilled over into other facets of our daily lives: driver’s license applications and renewals, utility and parking ticket payments, and collection of electoral and census data, to name a few examples.
Digital health care landscape in Ontario
The Ontario government, not unlike businesses, international organizations and other governments, has recognized the importance and value of information and communication technologies to inform and advance patient care, so it has invested heavily in health care digitalization. Investments have gone to:
- eHealth Ontario (formerly Smart Systems for Health Agency), the agency reporting to the Ministry of Health and Long-term Care (Ministry), for core infrastructure projects such as the provincial electronic health record (EHR) system, and data repositories for information such as diagnostic imaging and laboratory test results;
- Ministry-funded organizations and initiatives such as health care practitioner electronic medical record (EMR) adoption supported by OntarioMD, and for the Ontario Telemedicine Network, and Panorama; and
- Organizations funded through Local Health Integration Networks (LHINs) such as hospitals and Community Care Access Centres (CCACs).
Health care providers: an all-encompassing term used to describe an individual or a group who provide health care services to patients, for example, diagnostic technicians, or phlebotomists who draw blood samples. Other health care providers include physicians, nurse practitioners, and nurses.
Health care practitioners: refers specifically to two sub-groups of providers who are licensed in Ontario to treat patients - physicians and nurse practitioners.
Community physicians: primary care physicians (i.e. your family doctor) and specialists located in the community (i.e. not in a hospital), either in an individual or group practice.
These investments have provided us the foundational digital health system building blocks that we have today and will enable connections between health care providers, practitioners, and organizations, as well as opportunities for technological innovation and commercialization in the years to come.
Digital health resources – or what we refer to as digital health assets – are currently used to do many things: to give health care providers quick access to patient health information and medical histories, and to share, for example, diagnostic imaging and laboratory test results between community and regional health care providers.
Ontario has a large and complex system of digital health assets. Many health care providers use information systems at the point-of-care – meaning at the time and place of patient care – such as the EMRs that physicians and nurse practitioners use within their practices. These systems have been built and adopted in a disparate manner over the years. Different health care providers, organizations, and IT vendors have put them in place to support local needs, often with limited or no integration with the broader sector. That said, over the years, eHealth Ontario and its partners have built an integrated and foundational province-wide EHR infrastructure, made up of the connected backbone, data repositories, and viewers for health care providers to access shared patient information. An EHR constitutes an integrated history of a patient’s health care encounters that is available to authorized health care providers. Connection of the various systems used at the point-of-care with the provincial EHR is still underway. These systems and information flows are all governed by provincial privacy legislation and anchored by solid privacy and security protocols.
Over the years, eHealth Ontario and its partners have built an integrated and foundational province-wide infrastructure know as the province’s EHR system which includes a connected backbone, data repositories, and viewers. Connection of the various systems used at the point of care to the EHR is still underway.
eHealth Ontario
eHealth Ontario – an agency of the Ministry of Health and Long-Term Care (Ministry) – began its current mandate in 2008 and was the successor to the former Smart Systems for Health Agency (SSHA). Over the lifetime of these agencies, technology has moved a long way from the original core digital health care system model that was envisioned. In the early 2000’s, decisions about core infrastructure reflected available technology and the prevailing design trends and models at the time. It would have been impossible for anyone to predict where technology would take us and how much it would change in these years.
eHealth Ontario has played a key role as a builder and operator of digital health assets and systems, connector of information, facilitator of best practices, and provider of electronic services, which has provided tremendous support to other areas of the health care system. eHealth Ontario is not, and has never been responsible for all aspects of digital health in Ontario. The Ministry has responsibility for setting health care and digital health policy and direction for the Province of Ontario (Province), as well as for operating some systems that are not already operated by individual health care organizations and delivery partners such as the Narcotics Monitoring System. Many health care providers, patients, and the general public do not seem to be aware of this important distinction or other distinctions, such as definitions and specific terminology used to describe digital health care. As a result there is often confusion in discussions. For example, there are different understandings and interchangeable use of many terms, including:
- e-health initiatives (referring generally to the digitization and digitalization of health care);
- eHealth Ontario (the specific legal entity that is an agency of the Ministry);
- Electronic medical records (referring generally to digital records specific to one health care practitioner’s practice or organization); and
- Electronic health records (referring generally to the digital collection of a person’s health care encounters throughout the health care system).
eHealth Ontario has also been plagued by the troubled past of the former SSHA, which has included:
- Lack of operational stability with its management team and in the scope of its mandate and operations;
- Misunderstanding of its operational scope based on previous perceptions;
- Little agency leadership or accountability to provide system direction or to manage issues without the guidance or approval of the Ministry;
- Communication and cooperation issues with system partners, the Ministry, and other stakeholders; and
- Multiple reviews and media criticism about its management practices, finances, and reliance on external consultants.
Since 2009, eHealth Ontario has reoriented and transformed its leadership team, organizational structure, culture, and mandate, making it a different organization today. In 2014 a new CEO was put in place, and since then the management team has changed significantly. Graham Scott noted in his submission “under the leadership of the new CEO, the agency has addressed the validity of the past criticisms and has implemented the necessary changes since her appointment.” Unfortunately, the agency still carries a reputational burden from past difficulties. eHealth Ontario is a critical institution in the digital infrastructure of Ontario’s health system. It has many projects that need to be rolled out in the next two years. It is important that it be supported to do so.
The experts that I spoke to generally agreed that the infrastructure established by eHealth Ontario and the assets that other health care providers and organizations have built and implemented have advanced the quality of patient care in individual health care settings and within communities and regions. But most experts acknowledged that we can do more to increase quality by connecting more systems and getting more health care practitioners to adopt and effectively use digital health care technologies, always while respecting patient privacy and ensuring the security of personal health information.
They also agreed that it would be helpful to clarify eHealth Ontario’s mandate.
Digital health assets in Ontario
What are the digital health assets that have been created?
Recognizing the time constraints for my review, the following set of descriptions does not constitute a complete list of all of the digital health assets in the province. For example community mental health and addictions information systems and other community support services systems are not included.
- Electronic Health Records (EHR) viewers
eHealth Ontario supports two EHR “viewers” in three regions across the province, with 85,000 health care practitioners registered to use the viewers, but only a portion who are actively using them. Every month practitioners access over one million patient records. Both viewers also have their own way of accessing data, but eHealth Ontario manages the province’s core data repositories such as digital imaging and laboratory test results.
- Connecting Ontario in the Greater Toronto Area (GTA) is the provincial viewer that eHealth Ontario is building, and to date it has largely connected acute and community care organizations, and a) Community Care Access Centres CCACs in the region. The Northern and Eastern regions will be onboarding over the next year.
- ClinicalConnect in southwestern Ontario was developed as a regional solution while the provincial viewer was being designed and built, and it has been adopted by all hospitals and CCACs in that region.
It is important to understand how these two systems grew up. ClinicalConnect started as a practitioner-friendly way for hospitals in southwestern Ontario to access information from one another’s systems when patients received care at more than one hospital. It developed at a time when broader provincial solutions and repositories were not available from eHealth Ontario. Over time, ClinicalConnect was extended to include users and data from more hospitals in the region, as well as from health care providers beyond hospitals. It is now also beginning to incorporate key province-wide repositories built by eHealth Ontario. Connecting Ontario began in the GTA, providing access to shared provincial and regional health data repositories within and well beyond hospital settings. Some of the provincial repositories are the same as those available through ClinicalConnect, but some are different. Patient access to information from both systems is limited at this time.
Thus, while both systems have value within their own regions and there is some overlap in content that can be accessed through them, neither the viewers nor all of the underlying data systems are inter-operable, which means that most information cannot be exchanged or viewed between the systems or regions. In the short-term, energy spent arguing the merits of the two systems seems a waste of time. Rather, the focus should be on supporting both systems for the moment and commissioning an independent architectural review to help shape the path forward in the longer term.
Such a review of the ClinicalConnect and Connecting Ontario systems should determine if and how the systems should be connected and whether the best features of each system could be incorporated to form a hybrid system model. Any electronic health record system for Ontario must meet the following four requirements, as identified by experts:
- The ability to proactively and securely contribute patient information so that it is available to patients and to other health care providers in a patient’s circle of care;
- The ability for authorized health care providers to pull patient information from the EHR as needed (e.g. being able to access information in an emergency situation), ideally in a way that is seamlessly integrated with electronic medical records and other local point-of-care systems;
- The ability to access de-identified data from the system to support overall quality improvement, research, and other authorized secondary use that is consistent with the province’s privacy legislation and protocols; and
- The additional ability (with appropriate patient consent) to use patient specific integrated data to benefit the patient and to enhance population health by checking if necessary follow-up procedures were done and sending electronic reminders for critical lab results.
- Electronic Medical Record (EMR) systems
EMRs are point-of-care computer-based medical record software platforms used in community-based physician and nurse practitioner offices and similar organizations, which enable practitioners to provide better-informed patient care. Eleven software vendors have multiple platforms and offerings approved for use in Ontario. Currently, over 80% of community-based primary care physicians have EMR platforms. Getting EMRs into practitioners’ offices is an important milestone. Now the focus must be on increasing active usage. OntarioMD estimates that practitioners’ active use in Ontario is currently measured at a level two on their EMR maturity model, with level zero on the scale being paper-based record use and level five on the scale being integrated care using digital platforms and EMRs.
Because of gaps in active usage, not all Ontarians can count on receiving the full benefit that digital health care offers today. For instance, about one in five community-based physicians are still using paper records in their practices. Meanwhile, use of digital systems in hospitals varies widely, and a number of community (private) laboratory and imaging facilities are not making test results available to clinicians electronically.
OntarioMD EMR maturity model
Source: OntarioMDLevel Criteria Capabilities 5 Integrate Use of portals, hubs, attachment to provincial e-health platforms sharing data from the EMR. 4 Population data use Dashboarding of whole populations, acting upon the whole, performing population analysis at the practice level. 3 Look Ahead / Predict Reminders and alerts are used at the point-of-care. Searches are done regularly and scheduled for review. 2 Early data use Acting upon the output of episodic searches, quick entry tools, forms, calculators, etc. 1 Enter data Documentation occurs electronically. Progress notes, forms, and other documents are entered into the EMR. 0 Paper Processes are primarily paper-based. Although EHR adoption is not complete, and the extent to which EHRs and practitioners’ point-of-care EMR systems are actively used to support patient care varies, the good news is that health care practitioner adoption and active use is on the rise. Since 2013, the number of active EHR users in Ontario has grown significantly, with 34,637 active users reported in 2016.
Number of Active EHR users* in Ontario
Source: Canada Health Infoway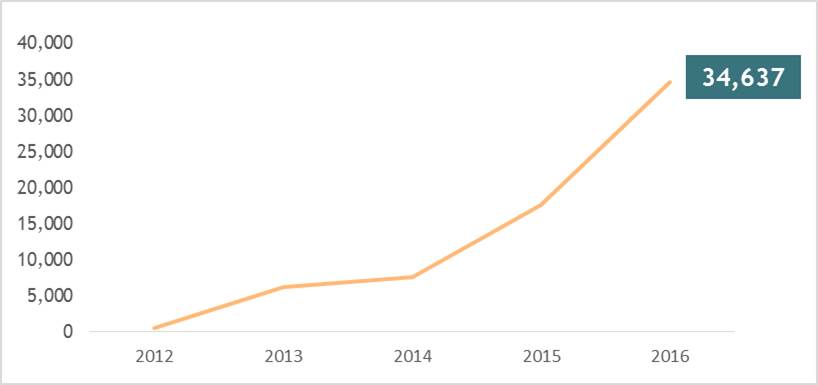
*Number of active users with monthly access to 2+ clinical domains.
Experts believe that active use will continue to grow as more systems are connected, more data becomes available, and practitioners gain experience with the use of these solutions to support patient care.
- Other information systems and data repositories
In addition to EMR, several other electronic systems are enabling clinical workflow and virtual, online care processes. Some of these systems connect to one another, and some connect into the EHR, but not all systems can draw information out of the EHR. Some key examples of these systems include the following:
-
Hospital Information Systems (HIS) are hospital-based information systems used to manage patient medical records and support patient care. They are now used in most hospitals across the province but in different ways. In some regions, HIS systems are connected to other health care providers, practitioners, and organizations within the community. For example, the North West LHIN has connected all 13 of its hospitals to the regional HIS, further improving access to hospital-based patient information for authorized health care practitioners.
Hospital organizations made their original HIS investments independently from government or eHealth Ontario. Although these systems have created value within their organizations, especially in the way of quality improvements and efficiencies through automation, these systems vary between hospitals and levels of investment, capacity, maturity of implementation, and benefits realized by way of internal efficiencies. Patient outcomes also vary from hospital to hospital. Other issues that have been identified include duplication of efforts and resources, and internal lack of standardization with respect to data collection and clinical protocols.
I was glad to learn through my engagement with the Ministry that a HIS renewal project, led by the Digital Health Board within the Ministry, is underway. This project will see hospitals organize into clusters or hubs when undertaking HIS renewal, to maximize the value of current and future investments. The long-term vision for these recommendations is that these digital health service hubs open up assets and capacity to include other health care providers within the community (e.g. community-based physicians and specialists). It is an approach that could help us to get the last miles built, and I encourage the Ministry to accelerate their implementation planning for this, and perhaps consider if additional funding is required to support implementation.
- Hospital Report Manager (HRM) is an electronic system that enables practitioners using approved EMRs to securely receive patient reports (e.g. discharge summaries, transcribed diagnostic imaging results) electronically through their EMR from participating facilities – primarily hospitals. In the short time since its implementation, over 6,500 physicians have started receiving HRM reports from over 175 hospital sites and specialty clinics, with numbers increasing by the month.
- The Ontario Laboratories Information System (OLIS) captures 91% of all lab test results entered into the system from all public health laboratories, 96% of community (private) laboratories, and results from most hospital laboratories. But health care practitioners with certified EMRs are not all connected to the system yet (though the technical capability is there to do so. But progress is being made. Last year, practitioners viewed 138 million lab test results for their patients, and viewing capability of these results is expected to grow in the coming years.
- A Drug Information System (DIS) captures nearly 70% of all drug dispensing interactions in its system, primarily for patients receiving drug benefits from the Ontario Drug Benefit Program or Trillium Drug Program through the Drug Profile Viewer. This information on publicly-funded medications is fed into the DIS from pharmacies through their point-of-care Pharmacy Management Systems. Health care practitioners are not currently able to widely access information on all patient prescriptions. However, efforts are underway by the Ministry to enable practitioners in some parts of the province to view this data in 2017. Planned access to drug information would be useful in managing patient care and would likely encourage more active EHR and EMR use.
- The Clinical Data Repository is the provincial repository built and operated by eHealth Ontario for sharing acute and community clinical information from hospitals such as discharge summaries, patient assessment forms, clinical notes, and transcribed reports or procedure reports. This repository also connects to all the other information repositories (such as labs, imaging, drugs, and immunization) allowing for an integrated set of patient specific data. The repository provides access to patients’ EHR information anywhere in the province and enables the additional ability (with appropriate consent) to monitor their health status and care (for example to ensure that all diabetics are offered annual eye examinations, checking if necessary follow-up procedures were done, and sending electronic reminders for critical lab results).
- The recently established Narcotic Monitoring System provides electronic data on all opioids prescribed by practitioners and dispensed by pharmacies anywhere in the province. The Narcotic Monitoring System has an important role to play in addressing opioid drug addiction and excess prescribing – an urgent public health crisis in Ontario and in other jurisdictions.
- The Client Health & Related Information System (CHRIS) is a secure web-based application and the core patient care system that is used by all 14 CCACs to connect the home and community care sector. CHRIS can also connect with other health care provider information systems in the community and with the Connecting Ontario and ClinicalConnect systems. Many CCACs also use value-added services such as electronic referrals and notifications for patients.
- Panorama is a system that provides public health officials with a way to manage immunization information, vaccine inventory, and cases and outbreaks of communicable diseases. Focus to date has been on capturing immunization records for school-aged children. Efforts are underway to expand the system to capture data for all Ontarians.
- The Ontario Telemedicine Network (OTN) operates an online videoconferencing portal that enables health care providers to interact with patients remotely. Telemedicine services were provided to 637,293 patients in 2015-16, more than double the number of patient services provided since 2012-13.
- Four Diagnostic Imaging Repositories (DIR) are in operation as part of eHealth Ontario’s Diagnostic Imaging Program. Diagnostic images and reports for X-rays, CT, and MRI scans are captured, viewed, and shared in all hospitals in Ontario. 40% of independent health facilities currently capture and share this data, but more independent health facilities are expected to come online over time.
-
These viewers, systems, and repositories are at different levels of technological maturity and different levels of inter-operability. Although these systems provide immeasurable value for the practitioners and patients who currently benefit from their use, powerful opportunities to advance and improve quality of patient care will only be realized when last mile connections are made and information is able to be pushed into the EHR, pulled out of the EHR, and moved between EMRs and the EHR, as needed by patients and authorized health care practitioners.
Differences across systems create challenges for connectivity and inter-operability, which ultimately affect the connection of last miles. There are vast differences between the systems in Ontario’s hospitals. There are different systems, some better than others. There are different levels of quality in the servers and the software used. And there are even differences in the extent to which hospitals have inter-operability within their own hospitals and have cyber-attack defenses.
There are also important differences in the degree to which systems are integrated and adapted to practitioners’ workflow, which affects the degree to which they support the delivery of safer, more seamless care to patients. Hospital systems are one of the key last miles. Other key last miles include those for community-based physicians and specialists, nurse practitioners, and home and community care providers working outside of hospitals.
Again there are different EMR software platforms being used. Some EMRs are better than others. There are different degrees to which health care practitioners use their EMRs as the main patient record and to support patient care services (e.g. reaching out to patients overdue for recommended preventative/follow-up care and connection to health care providers online). And there is very limited use of their EMRs to share with and receive information from others on the care team.
In addition, there are major last miles to be completed including patient-facing online resources – including consideration for the requirements of diverse communities such as Franco-Ontarians and Indigenous peoples – so patients can see their own health records.
Examples of upcoming activities
I am struck by how Ontario’s digital health progress is a classic glass half full / glass half empty situation. By this I mean that tremendous progress has been made to date, but such progress also underlines the need to do more, faster. We have come so far, yet we still need to make many last mile connections that would realize greater value for Ontarians. But as you will read, we are on the verge of making more progress and we can do more.
eHealth Ontario
As part of my engagement with experts, I asked eHealth Ontario where they think they are today and where they are heading, and I was happy to hear that the benefits of past investments are coming online as digital health care continues to expand. For example, drug data will be made more available to health care practitioners in 2017 and information from community-based physician’s offices is expected to be added to the electronic health record (EHR) system’s data repositories in 2018-19. This information will also become progressively more valuable provided that practitioners' active use of their electronic medical records (EMR also continues to grow.
Additionally, eHealth Ontario is beginning to focus on innovation and new partnerships. In its submission to me, eHealth Ontario acknowledges the need to involve the private sector in the evolution of Ontario’s health care digitalization, so as to provide patients with all the advantages that evolving technology can provide in managing their own health care, and to arrive at a truly user-friendly system. An example of this is the launch of a digital health Innovation Lab at Mohawk College in April 2016. Innovators and solution providers can now test their apps and solutions in a formal testing environment. eHealth Ontario notes that the lab provides an opportunity for more companies to enter the digital health market and that it will help vendors who want to respond to procurement requests to better understand risks and costs. The idea behind the Lab is to encourage experimentation to help produce innovative technologies and apps aimed at helping individuals live healthier lives and prevent the onset of disease.
Ministry of Health and Long-Term Care
From my engagement with the Ministry, and from reviewing their written submission to me, I understand that the Ministry has made progress to date in developing a renewed digital health strategy. I look forward to seeing how the Ministry will chart a path forward that leverages our current digital health assets. I understand that a new strategy will include a number of new initiatives under the governance of the Digital Health Board that reports to the Minister of Health and Long Term Care. This Board was established to develop a strategy and provide direction for digital health services across the province. I understand that 850 clinicians, digital health experts, patients, and other health care service providers have contributed to this work. I think these initiatives, when underway, will do a lot to further eHealth Ontario’s work and the connectivity of our system. And I hope progress will be made quickly on Hospital Information System (HIS) renewal and increased health care practitioner access to drug information, as mentioned earlier.
As we make more and more of these systems available to health care practitioners and to patients, and as we increase the connectivity between all of our systems in a privacy-sensitive way, we should see greater use of the infrastructure that we have built. Late adopters of these systems will both want and need to come on board and actively use them, either to continue providing the best available care in their practices or because their patients demand it, or both.
How much value has been created by efforts to date
As I referenced earlier in my letter, value can be defined and calculated in many ways. For the purposes of this assignment, I have assessed the value of our digital health assets in five ways. These categories can be used to assess both the value of current assets and the potential of these assets:
- Producing better clinical outcomes: better quality of care (e.g. safer prescribing of medication) and more informed treatment options;
- Improving patient experiences: less stress (easier and quicker access to knowledge of results, simpler ways of tracking immunizations), with less wear and tear (fewer repeat tests and appointments) and more access (less travel time, and elimination of unnecessary referrals);
- Reducing health care system costs: creating efficiencies, including by avoiding repeat or unnecessary procedures and ensuring patients in need get the right help sooner (telehomecare);
- Enabling data analysis to improve the quality of health care: patient-centric research to find more effective ways to meet patients’ needs; and ensure (with the patient’s consent) that they are getting the right care; and
- Stimulating economic growth: creating an environment where innovators can create new health system products in Ontario and market them both to our health care system and to others around the world.
According to the Conference Board of Canada, there is a significant return on investment from digitalization. Investments made as a result of the 2010 federal grant to Infoway add about $1.48 to overall GDP for every $1 invested. This is good news from a growth and jobs perspective, and it shows that the large investments provinces have made and continue to make across the country are making a difference for our economy.
Here’s an example of how my wife used these tools to achieve a good outcome at low cost with high quality.
She experienced a few weeks of an elevated heart rate, unintended weight loss, and brittle hair - all symptoms of thyroid disease. She used the Beth Israel Deaconess secure texting application to develop a care plan with her primary care giver. The first step was a set of thyroid function tests at a local lab 5 minutes from our home. Those results were sent by the lab to an app on her phone and within hours we confirmed she was hyperthyroid. She used the patient portal application to set up an appointment with a specialist the next day at a location a few minutes from our home. At that appointment she was diagnosed with Grave’s disease and the clinician electronically prescribed Methimazole to a pharmacy 50 feet from our home. My wife walked to the pharmacy and now a few weeks later, she’s symptom free.
Dr. John Halamka,
International Healthcare Innovation Professor at Harvard Medical School and
Chief Information Officer of the Beth Israel Deaconess Medical Center
This past summer a family member who lives in Hamilton, Ontario needed to go the hospital while on vacation in Goderich Ontario. He has a number of health related issues so he packed up all of his medications into his grocery bag and headed off to the hospital. To his delight and pleasure, when he arrived at the hospital he was told that they had access to all of his medical records through Clinical Connect. They could even access his recent x rays and lab work.This meant that blood work and x rays (and potentially other tests) did not need to be repeated. The physician did not need to spend time trying to puzzle together his history. It meant that my family member received safer care in a more efficient manner and it cost the health system less as he didn't need to have tests that had already been done, repeated.
With all hospital and home care information connected in the south west area of the province through Clinical Connect repeating unnecessary diagnostic tests is a thing of the past.
Donna Cripps,
Chief Executive Officer, Hamilton Niagara Haldimand Brant Local Health Integration Network
In 2012, a patient in south west Ontario was hospitalized for a severe reaction to an antibiotic. She was rushed to hospital, where she spent a week in the intensive care unit on the brink of kidney failure. After recovering, the patient was discharged home a week later. However, it was just a few days before she was readmitted to hospital with another infection – and the care team tried to prescribe the same antibiotic she had just reacted to. Today, the patient receives care from specialists as well as their primary care physician.
Digital health systems such as ClinicalConnect contain patient medical information, including allergies, which helps reduce risk of adverse drug reactions. And because members of the patient’s health care team, whether in hospital or the doctor’s office, can securely access information about previous health events, they can coordinate the patient’s care, such as reducing repeat lab and diagnostic tests, and improve the patient experience.
Murray Glendining,
Connecting South West Ontario Program – Co-Chair, Steering Committee
President & CEO, London Health Sciences Centre
MyChart, an example of a personal health records system, empowers the patients so much more – like we are in it together. And it is a whole new way of doing medicine.
Patients can see when their test results have been completed and can then initiate a follow-up appointment. And when several doctors are given access to the patients records, there is less of a chance that tests will be duplicated. So MyChart has the potential to speed up treatment, while saving the healthcare system money.
Dr. Barry A. McLellan,
President & CEO, Sunnybrook Health Sciences Centre
How to measure the benefits
There is no simple way to establish what benefits were created by our current digital health assets. We have to look at several different studies to get a comprehensive view. A starting point has to be Canada Health Infoway (Infoway).
The Government of Canada established Infoway to both promote digitalization of health care systems but to also monitor progress at the national level and across the provinces and territories.
Ontario is well positioned relative to its peers in terms of availability, use and benefits from investments in digital health solutions.
Canada Health Infoway
They have published or sponsored a number of studies on the benefits of health digitalization. An important study is the annual estimate of progress being made across Canada. We were able to obtain a provincial breakdown of their data for Ontario.
Infoway would underscore that their data represents a partial valuation of the benefits. They do not include benefits under our last two categories of value (data analysis and economic growth) although they have sponsored work in both areas, and believe there are important benefits there (see insert from Jennifer Zelmer). As to the other three categories of value, they would capture only part of the benefits.
Independent studies commissioned by Infoway have tracked access, quality, and productivity benefits valued at billions of dollars since 2007. These studies focused on specific types of health IT: digital diagnostic imaging, drug information systems, electronic medical records, and telehealth. Health IT solutions not yet studied in this way – such as laboratory information systems, public health surveillance systems, and clinical systems in hospitals – likely generate additional value. Also, not all that counts can be counted. Some benefits, such as peace of mind from earlier access to test results, cannot readily be translated into monetary terms and so are not reflected in the studies’ estimates.
Jennifer Zelmer,
President, Azimuth Health Group and previous Executive Vice-President at Canada Health Infoway
Infoway’s estimate of value includes the benefits realized through:
- Digital imaging (2008)
- Drug information systems (2010)
- Telehealth (2011)
- Electronic Medical Record (EMR) use in community-based clinics (2013)
- Telehomecare (2014)
- EMR use in hospital-based ambulatory clinics (2016)
Infoway cites several examples of systems and services enabled through digitalization that are not captured in pan-Canadian benefit evaluation studies commissioned by Infoway. These include:
- Clinical and health system analytics
- Clinical synoptic reporting
- Community care information systems
- Disease-specific registries
- eBooking
- eConsult
- eNavigation
- ePrescription renewal/refill
- eReferral
- eVisit
- Hospital information systems
- Laboratory information systems
- Long-term care information systems
- Patient flow management
- Patient portals/eView
- Public health surveillance systems
- Telepathology
- Wait times tracking systems
For Ontario specifically, this means that systems such as the following are not captured in Infoway’s benefit calculations:
- Ontario Laboratories Information System (OLIS)
- Cancer Care Ontario
- Panorama
- Community Support Services
With these caveats, what do the Infoway studies tell us? Ignoring the benefits not included, in 2015-16 Ontario’s digital health assets generated annual benefits of $900 million per year. To put this into context, the Ministry of Health and Long-Term Care would estimate that their spending on digital health assets, including on systems not covered in Infoway’s valuation of benefits, was just under $900 million in 2015-16. If we included all the benefits not counted, the extent to which benefits exceed costs would be quite large. In short, our investments in digital health have brought us to a point where the ongoing value created significantly exceeds the Province’s cost to maintain and grow our digital health assets. This is a major milestone.
It is obvious that we have created huge potential value. The analogy that I used earlier about highways is a perfect example. Our experts told us that if we can just continue to build the ramps and feeder roads that connect onto the highway, the value of our previous investments will increase drastically.
We can use the same Infoway study to get a sense of a cumulative minimum value over the years. For Ontario, Infoway’s written submission put the value for the period of 2007-2015 at $5.7 billion (in constant 2015 dollars). A big number, but again it is worth noting that it is only a partial estimate – the true valuation would be significantly higher.
Infoway’s latest independent performance evaluation published in spring 2016 notes that Infoway has:
- Been a leader in benefits evaluation, at the project level where it is a requirement of many projects, and at the higher jurisdictional and pan-Canadian levels.
- Worked with stakeholders to develop and evolve a Benefits Evaluation Framework that has been used for many years to standardize benefits evaluations. The evaluations show benefits in access, quality and productivity, within investment programs.
Infoway also received the 2014 Canadian Government Executive Leadership Award in recognition for its continued commitment to accountability for investments and excellence in project management.
How Does Ontario Compare to Others?
According to Infoway, Ontario is also leading the way in many of its digital health care efforts compared to other provincial jurisdictions:
- Ontario has been among the leaders in EMR adoption, and compared to other provinces, Ontario is making rapid progress in the growth of practitioners using EMRs;
- Ontario’s early establishment of its EMR program accelerated community practice adoption in Ontario;
- Ontario is leading in both Telehealth and Telehomecare, and enrolments in Ontario have led Canada in volume and growth; and
- Ontario is a leader in digitizing diagnostic imaging.
I also sought outside expertise on where Ontario ranked in the world. Dan Sheldon confirmed that in his view, Ontario is ahead of other jurisdictions in specific digital health assets, such as diagnostic imaging. But he notes that Ontario (along with the rest of Canada) still lags significantly behind the United States in HIS adoption, but we are seeing incremental improvements.
He also notes that other countries have struggled with implementing digital health care, and have had multiple setbacks, and that no single health system is close to delivering all of the building blocks of health care IT.
- England has failed to deliver a national patient record system and in 2014, it launched a new digital health strategy including directing the Nhs Digital agency with its delivery by 2020. Key issues that impacted the delivery of a national patient record system included inter-operability and fragmented HIS adoption, as well as limited availability of digital service offerings for health care users.
- Australia has not been able to deliver on its national personal health record service due to low adoption and poor clinical engagement. The government has established an agency to improve on the service and a new digital strategy is expected to roll out in the near future.
The key take away from these examples is that despite large-scale failures, these jurisdictions see value in the infrastructure that they already have in place, they are continuing to invest in their digital health care systems, and they are pushing on with the delivery of this work.
Conclusion
Ontario has created digital health assets of significant value. It has crossed an important milestone of creating more value than it costs, including costs involved in adding further value. It has huge potential value, and compares well with other provinces.
Key themes
To inform my review and recommendations to government, I heard from more than 30 expert individuals and groups, and asked 33 of them to produce a short submission on how they would describe their perceptions of digital health assets and their associated value. The level of enthusiasm that I observed among experts on this topic is a good indicator of how organizations and agencies are open to communicating, collaborating, and coordinating with each other if provided the opportunity to do so. Below, I highlight the key themes that emerged through the course of my engagement with experts.
- Experts welcomed the opportunity to openly express their views and to review the input from their peers on this topic. They care deeply about the system, and are anxious to ensure that we continue to make progress in digitalizing health care.
- Regardless of individual perspectives on the state and progress of adoption of digital health systems in Ontario, there is a strong consensus that the ever-increasing digitalization of the health care system adds or enables enormous value in a variety of ways, including:
- producing better clinical outcomes;
- improving patient experiences;
- reducing health care system costs;
- enabling data analysis to improve the quality of health care at the individual and population health level; and
- stimulating economic growth.
- There has been considerable work done by Canada Health Infoway to estimate the value created by digitalizing health care in Canada. This work indicates a strong growth in value created over time. Based on the Ministry of Health and Long-Term Care’s analysis, with Canada Health Infoway inputs and verification, about $5.7 billion in benefits were realized across Ontario from 2007 through 2015 from investments in digital imaging, drug information systems, electronic medical records, and telehealth alone. Of this, $900 million in benefits were realized in Ontario in 2015. These estimates clearly understate the total value created. Almost everyone we talked to provided examples of improved patient care or lives saved, many of which go beyond areas where value could be quantified in Canada Health Infoway’s studies. Use of hospital, immunization, home care, laboratory, and other information systems also created significant value that is not captured in these estimates. In addition, it is clear that as work proceeds – to improve repositories, add users, or broaden the way data is used to support patient care – value increases significantly.
- According to the Ministry of Health and Long-Term Care, a rough estimate of what Ontario is spending to obtain benefits on health IT would be just under $900 million in 2015-16. Using a narrow definition of benefits, benefits are now exceeding costs. This is a major milestone.
- Experts were strongly of the view that if you stepped back and looked at the total value created, the benefits of digitalization clearly exceed the costs. They backed up their views with many examples of value creation and cited examples of how they had made decisions to divert limited funds to speed up digitalization because of their belief in resulting value. Experts also urged that more aggressive and ambitious targets should be put into place to push forward the full digitalization of our health care system.
- A number of experts underscored the dynamic nature of technology. It is not only an enabler – it can also transform practice protocols. Digital health care solutions can improve health care in ways we have never imagined. Health care providers should be aware of how technology can help them improve the care they provide to their patients and we should encourage the effective adoption of new technologies. A key part of digitalization will be ensuring that key policy enablers are in place, and that health care providers feel appropriately supported as they embrace digital systems and tools in providing high-quality, accountable, and modern patient care.
- Experts encouraged a sense of urgency for increasing connectivity with patients, but acknowledged that this work would not be without challenges. Experts also noted that the requirements of our diverse communities should be considered when undertaking this work. Patients should have real time access to their own electronic health records and online services, including through secure, convenient and technologically relevant channels such as patient-facing online resources and smart applications. Understandably, digital health systems to date have been designed primarily for use by health care providers. Giving patients the ability to see their own health information and interact with their health care team online will demand changes in attitudes and user interfaces to enable patients as users and verifiers of their information. Patients themselves are motivated more than anyone else to ensure that their health information is accurate. They will also be a source of pressure to bring the health system up to the standards of other industries in allowing digital access.
- There is an extraordinary understanding among experts I spoke with about how the digital landscape has evolved over the years, what has worked and not worked, and of key issues, system obstacles, and underlying complexities that prevent realizing additional benefits from Ontario’s digital health assets. The complexity and governance of the health care system also make it difficult to execute discrete solutions and larger overall strategies. Adding to this complexity is Ontario’s permissive approach to delivery and implementation of digital health solutions, which has resulted in positive innovations but also in increased system complexities. Based on what we have learned from efforts across the province, we are now in a position to identify proven solutions that should be widely adopted. To better plan for mature system use, a coordinated province-wide strategy, and improved last mile connections, we must start being more directive about system delivery and implementation and we must do so in a thoughtful, evidence-informed way that still allows for openness and competition between vendors within the health care system. We must also draw on and apply the experiences and lessons we have learned along the way. A shift from a permissive to a more directive approach can help ensure that all patients benefit from more modernization in the health care sector. When health care practitioners aren’t sharing with and using data from their colleagues, there is a risk that their patients may not receive the best possible care.
- Building on the concept of improved last mile connections, experts generally agreed that many IT systems and software applications are neither as inter-operable at this time as they should be, nor is shared information governance as well-established as it needs to be. This means that even if a patient gives full consent for their information to be shared between health care providers, systems sometimes still can’t talk to one another, and general inequities in quality of care can result, leaving individual patients behind. While Ontario’s policy approach has been to not be directive about the need to achieve end-user performance standards and system requirements, it is time to begin doing so. While the Province of Ontario’s permissive approach has resulted in multiple systems – we should not do away with those systems, rather we should improve upon them. As a start, Local Health Integration Networks already have a responsibility for hospitals in their regions, and so they should begin to phase in minimum standards for connectivity, inter-operability, and performance moving forward, which would improve the experience of patient care.
- The growth in different platforms, patient-facing online resources, and viewers has led to a spectrum of different contractual arrangements between various health care sector entities and their respective vendors. IT vendor management is not typically a core competency for health care providers. With no centralized source of expertise, each agency or practitioner is left on their own and, not surprisingly, this tilts the playing field in favour of suppliers and vendors. Efforts should be made to leverage economies of scale from vendors and to find ways to encourage best practices.
- Experts agreed that ensuring the safe and private handling of patient information is of central importance in our digital health care system. With increasing connectedness between various information systems and increased adoption of new disruptive technologies, especially in the primary health care environment, current security efforts, which have been focused on the protection of individual patient data, need to continuously be expanded and updated to ensure increased resistance to cyber-attacks.
- Many experts underscored the need to emphasize that they see nothing inherently wrong with competition between multiple vendors of technological solutions, but a framework is required to make expectations explicit for vendors, using a balance of appropriate enablers and regulatory measures to allow for coexistence between large scale enterprise systems and new innovative platforms that can unleash the specific skills and talent found in Ontario’s innovation hubs.
- There is general agreement that the opportunities provided by Ontario’s digital health assets can yield material and significant improvements in greater clinical effectiveness, improved patient outcomes, and reduced health care costs. It is also generally agreed that there is a need for a linkage to the innovation economy. The Province of Ontario will need a more directive and modern legal, policy, and procurement framework that would realize the potential of our innovation economy to contribute to health care innovation, yet ensure that the core values of the health care system and our existing patient privacy framework remain protected. The province has a natural competitive advantage in the innovation economy, and significant opportunities could be realized if the health care sector could be linked more closely with innovation hubs, such as those in Ottawa, Toronto, and Waterloo. The talent in these hubs would also quickly identify new possibilities for the Canadian economy if allowed to do so.
- Experts in Ontario’s health sector generally agreed that there has been no clear explanation of the strategy for digital health in Ontario, nor identification of links between a digital strategy and an overall strategy for health. The various roles and responsibilities with respect to the digitalization of Ontario’s health care system are unclear.
- eHealth Ontario, as an agency, has made progress towards the complete adoption of electronic health records, particularly in the last two years. Experts cited the mixed success of health digitalization in other jurisdictions. They urged us to focus on how to move forward. There is general agreement that the maturity of systems is still many years from completion, but that eHealth Ontario is well positioned to make significant progress in the next few years if it continues with the right focus. We can learn a lot from other jurisdictions as we make improvements to the speed, performance, and reliability of our systems. Experts indicated that this could be achieved by focusing eHealth Ontario’s mandate on core activities, establishing new partnerships, and looking at consolidating functions that are not central to the complete adoption of electronic health records in Ontario. Clear communication of eHealth Ontario’s progress to date, ongoing and regular updates about its future progress, and its renewed mandate would be valuable.
- eHealth Ontario’s ability to execute on the expectations that have been placed on it will require help. The agency does not have the ability to command Local Health Integration Networks, individual hospitals, and health care providers and practitioners regarding their own systems or how they use health information. Indeed, it is a common theme that it would not be appropriate to have the agency serve in that role. That direction will need to be provided from above the agency. Under current governance models, that responsibility rests with the Ministry of Health and Long-Term Care and regulatory bodies – and there is general consensus that to ensure fair access to quality care for patients across the province, governance models should gradually shift from a permissive approach, which can result in inequitable and uneven patient care across the province and leaving individual patients behind, to a directive approach over time, where the quality of patient care has the full benefit of proven connected digital health assets – once appropriate enabling technologies are completed.
Recommendations
Based on the key themes identified and informed by my engagement with experts from the health care sector, I present the following recommendations to the Minister of Health and Long-Term Care:
eHealth Ontario
- The Ministry of Health and Long-Term Care should explicitly recognize the clear value that eHealth Ontario continues to create for the health care system in the Province of Ontario as a builder and operator of IT systems, connector of health care information, facilitator of best practices in digital health assets, and provider of data services, which provides tremendous value to its partners in the health care system and to Ontarians.
- The Ministry of Health and Long-Term Care should re-scope the mandate of eHealth Ontario with an explicit focus on technology service delivery and to ensure the agency is held to account for delivery against its mandate. This mandate should recognize that while eHealth Ontario is a builder and operator of core IT infrastructure, it is not a governing body of hospitals and health care providers. It does not have the ability to override the decisions of individual hospitals, oversight committees, or Local Health Integration Networks, nor should it. eHealth Ontario plays a limited but vital service role in the larger world of digital health assets. Specifically, eHealth Ontario should:
- Focus on core activities, completing the connecting projects, and operating and sustaining them in a way that is consistent with industry best practices.
- Be held accountable for meeting specific targets, milestones, and timelines, as determined by the Ministry of Health and Long-Term Care, in support of its mandate.
- Work with its partners to provide strategic advice and technical guidance on connectivity and inter-operability between eHealth Ontario’s systems and other users of digital health assets.
- Work with the Ministry of Health and Long-Term Care and with clients and partners to establish clear service standards for the assets that eHealth Ontario manages, and to develop new accountability mechanisms to properly enable the agency to meet those standards. The agency should prioritize the ongoing development of a customer service culture in all aspects of its work and organization.
- Work with the Ministry of Health and Long-Term care to modernize its approaches to developing and setting inter-operability standards, consistent with Ministry of Health and Long-Term Care leadership and industry trends.
- In light of its re-scoped mandate, work with the Ministry of Health and Long-Term Care to clearly define budgetary targets, and performance measures including meaningful usage, and costs per use.
- In light of shifting eHealth Ontario to become more of a service provider:
- The government should consider the quality, skills matrix, and experiences of human resources required and for the eHealth Ontario Board of Directors.
- eHealth Ontario should enhance the skills and qualifications of its stakeholder-facing delivery staff roles to ensure they reflect the shift of the agency to being a service provider.
- eHealth Ontario should develop and measure clear metrics, informed by stakeholder feedback as appropriate, to manage the performance of front-line delivery staff.
- The Ministry of Health and Long-Term Care should develop key indicators to measure eHealth Ontario’s performance as a service delivery organization.
Digital health strategy
- The Ministry of Health and Long-Term Care should more clearly articulate an operationally driven digital health strategy for the province including links to broader health strategies. Emphasis should be placed on the roles, responsibilities, achievements and objectives of each specific actor in supporting that strategy, including the Ministry of Health and Long-Term Care, eHealth Ontario, hospitals, Local Health Integration Networks, health care providers and practitioners, research organizations, and other partners.
- In describing roles and responsibilities, the strategy should make it clear that the Ministry of Health and Long-Term Care is responsible and accountable for the overall vision of the strategy and it should assign sharp deliverables and timelines to specific actors and organizations and detail individual expectations in meeting specific objectives within the larger strategy.
- The digital health strategy should include a rolling vision for the next 7 years, including yearly key milestones based on the needs and experiences of patients and informed by learnings from other jurisdictions, to be renewed at its completion.
- The digital health strategy should also include, in addition to specific milestones and targets for electronic health records, specific defined expectations and minimum operational requirements around quality of data and inter-operability for electronic medical records, data repositories, and other digital health solutions used by health care practitioners.
- In developing these standards, the Ministry of Health and Long-Term Care should avoid creating a non-competitive environment for health information systems. It should encourage competition and ensure the system will allow new players and new technologies opportunities to challenge existing players.
- As part of the development of a digital health strategy, the Ministry of Health and Long-Term Care should work with eHealth Ontario to clearly define its role, approach, and plan for making data from the assets that it manages available to patients, consumers, and innovators.
- Through the digital health strategy, the Ministry of Health and Long-Term Care should work with its partners to confirm and communicate its targets for mature use of digital health systems, inter-operability, and connectivity, with preliminary goals of:
- Electronic Health Record goals:
- Within 5 years, all authorized care providers should be accessing and contributing to patients’ shared electronic health records so as to improve coordination of care.
- Electronic Medical Record goals:
- Within 5 years, 95% of community-based practitioners should be using secure electronic tools in their practices that enable them to keep patient records, to connect with their patients, to improve access to care, and to trigger evidence-based alerts and reminders (e.g. about medication safety or preventative and follow-up care).
- Hospital goals:
- Within 5 years, all hospitals should be using electronic tools to improve medication safety, to bring the latest clinical evidence to the bedside, and to share information with patients and those caring for a patient after discharge, in order to ensure more seamless follow-up care.
- Patient-facing online services goals:
- Within 5-7 years, all Ontarians should have online access to their own health information, such as test results, and to proven tools that enable them to book appointments, request prescription refills/renewals, connect with health care providers, manage their health, and share information as they choose to with others involved in their care.
- Electronic Health Record goals:
- The digital health strategy would emphasize the need to take a “digital health by design” approach to implementing the strategy. This means that when the Ministry of Health and Long-Term Care, Local Health Integration Networks or health care providers create new health policies or programs, they should specifically think about how to achieve their goals using modern technology and ask “How can we do it with digital health care?”
- As a first step in implementing a digital health strategy, the Ministry of Health and Long-Term Care should confirm its support of the recommendations in this report, release its digital health strategy paper in the next few weeks, and publicly commit to releasing a final digital health strategy and action plan within 4- 6 months that includes targets and timelines that respond to these recommendations, confirmation of 3-5 signature projects, and budget details to support implementation of the strategy. The Ministry of Health and Long-Term Care should also release the results of its engagement activities around strategy development to date.
Digital Health Strategy Secretariat
- The oversight of the digital health strategy should be assigned to one specific point of contact, a Digital Health Strategy Secretariat (the Secretariat) with an executive led by an Associate Deputy Minister / Chief Information Officer, and supported by two Assistant Deputy Ministers. The executive lead of the Secretariat would be accountable to the Deputy Minister of Health and Long-Term Care to ensure the full implementation of the digital health strategy. This Secretariat would be assigned additional authorities and powers to affect its mandate, including the ability to work with appropriate partners to move from a voluntary and permissive approach to a directive approach to the adoption of specific connectivity, inter-operability, and data standards over time including across multiple layers, sectors, and systems. The Secretariat would also be responsible for liaising and coordinating work with other areas of the Ministry of Health and Long-Term Care and government in order to complete milestones for the strategy and to identify and coordinate key linkages with broader health system strategies.
- Recognizing the necessary role of technology in improving patient outcomes, reducing health care costs, and supporting clinical effectiveness, the Secretariat should be able to direct that a percentage of dedicated funding in health care capital and operating budgets be allocated for IT system modernization and renewal, and upgrades to minimum standards.
- The Secretariat should also leverage existing IT committees and/or work with eHealth Ontario, health care sector Chief Information Officers, health care providers, other industry professionals, and patient and family advisory groups on ways to continuously address system issues and improve established standards.
- The Ministry of Health and Long-Term Care should ensure that dedicated funding to health care providers for IT modernization and renewal, inter-operability requirements, and upgrades to achieve these minimum standards are focused on enabling health care professionals to provide better care and/or empowering patients.
- The Secretariat should support the Digital Health Board, currently chaired by the Deputy Minister of Health and Long-Term Care on behalf of the Minister, and require regular reporting on implementation progress of the digital health strategy, including progress towards specific timelines, targets, and milestones. A major function of the Digital Health Board would be to regularly review the value of investments made by the Province of Ontario and use an evidence-based investment management framework to inform its decisions.
- The Secretariat should work with health care regulatory colleges, associations, and other partners to identify opportunities and incentives for health care providers and practitioners to improve care by employing new approaches for the adoption of and increased use of digital health technology, and the adoption of common standards relating to the input of patient data.
- The Secretariat should commission independent architecture reviews, now and on a periodic basis thereafter, to ensure that evolving plans for the province’s electronic health record assets reflect priority use cases identified in the digital health strategy, leverage digital health assets and capacity from across Ontario, and reflect best practices in architectural design to meet user needs and maximize value for money.
- The Secretariat and its support structure should be restructured from existing Ministry of Health and Long-Term Care resources and a sharper, more implementation driven focus, resulting in no net new costs to taxpayers.
- The design of the digital health strategy must include a focus on minimum requirements for last mile connections and end users such as health care providers, practitioners, and patients, who should have the right to access their electronic records in an accurate, fast, and secure manner.
- The Secretariat, working together with eHealth Ontario for electronic health records, Local Health Integration Networks, OntarioMD and other delivery partners, should set about a phased approach for increased standardization that would make requirements clear and easy to understand for vendors seeking to participate in the Ontario health care sector – including minimum requirements around data compatibility, security, performance and speed, inter-operability between systems, system flexibly to adapt to rapidly changing technology, and the provision of data and services directly to patients and consumers.
Digital access and experiences for patients
- The implementation of the digital health strategy must include a strong focus and set of minimum requirements for the patient experience including considerations for addressing requirements of diverse communities and measured and demonstrated improvements in patient satisfaction and outcomes. Patients should be able access their own electronic health records and access online services, including through secure, convenient and technologically relevant channels such as web-based and smart phone applications. The Ministry of Health and Long-Term Care should ensure the creation of an open architecture to support the creation of patient apps to allow innovation in the presentation of patient data while also protecting the privacy of patient data and the integrity of the system.
Centre of Excellence for Cyber Security
- The government should establish a Centre of Excellence for Cyber Security (the Centre) with appropriately skilled resources. The Centre should be responsible for maintaining and updating existing standards, and adopting the latest standards to ensure that cyber security keeps pace with increasing inter-operability. The Centre should also be responsible for sharing information, intelligence, and solutions to ensure that security of digital health systems is up-to-date. The Centre could be housed in either the Ministry of Health and Long-Term Care or somewhere else in the government (to serve as a Centre for all government cyber security provided doing so does not unduly delay its establishment and provided there is a specific focus on digital health assets). Specifically relating to Ontario’s digital health assets, the Centre of Excellence for Cyber Security should:
- Work with OntarioMD and vendors, health care provider Chief Information Officers, eHealth Ontario, and other users of digital health assets to inform its work.
- Make recommendations through Local Health Integration Networks (LHINs) to all LHIN-funded health care providers on areas that influence the connected network including data compatibility, security, performance and speed requirements, and inter-operability between systems.
- The Centre should also enable certification of systems or patient apps as meeting cyber security required standards.
Hospital Information System (HIS) Renewal Advisory Panel
- The Ministry of Health and Long-Term Care should accept all of the recommendations from the HIS Panel, including partnering hospitals when undergoing system upgrade activities and the extension of key system infrastructure out into the community to form hubs with other community health care providers and practitioners.
- The Ministry of Health and Long-Term Care should work with eHealth Ontario to acquire the resources necessary to undertake a detailed architectural review of the ClinicalConnect and Connecting Ontario systems to determine if and how the systems should be connected and whether the best features of each system could be incorporated to form a hybrid system model. Any electronic health record system for Ontario must provide the following four requirements, as identified by experts:
- The ability to proactively and securely contribute patient information so that it is available to patients and to other health care providers in a patient’s circle of care;
- The ability for authorized health care providers to pull patient information from the electronic health record as needed (e.g. being able to access information in an emergency situation), ideally in a way that is seamlessly integrated with electronic medical records and other local point of care systems;
- The ability to access de-identified data from the system to support overall quality improvement, research, and other authorized data analysis that is consistent with the province’s privacy legislation and protocols; and
- The additional ability (with appropriate patient consent) to use patient specific integrated data to benefit the patient and to enhance population health by checking if necessary follow-up procedures were done and sending electronic reminders for critical lab results.
Centre of Excellence on Procurement and Vendors
- The Secretariat should establish a Centre of Excellence on Procurement and Vendors (Centre of Excellence) to help health care practitioners, hospitals, and other users of digital health assets get the best possible contract value out of the numerous vendors currently offering various electronic health record and electronic medical record solutions. This Centre of Excellence could also be housed in a provincial government centre provided there was sufficient focus on health institutions and provided it did not unduly delay its establishment given the imminence of many procurement decisions in the health sector.
- The Centre of Excellence, in consultation with the Chief Health Innovation Strategist of Ontario, should provide advice and samples of best practices, develop approval guidelines and procurement policies that take advantage of the repetitive nature of health information systems implementation, leverage greater volume discounts, and ensure standards for security and inter-operability. Health care providers and hospitals should be encouraged to band together to leverage the greatest possible value from scarce resources.
- The Centre of Excellence should be funded from the savings that it will create, resulting in no net new costs to taxpayers.
Innovation
- The Province of Ontario should call on the federal government to support modernization and renewal of hospital IT infrastructure. The call from Ontario, preferably in collaboration with other provinces, should underscore that upgrades to connectivity and investments in big data produce ever-increasing positive economic returns and support the federal government’s Innovation Agenda.
- The Ministry of Health and Long-Term Care should work with its partners and with innovators to identify and provide alternative financing structures and innovative solutions to support investments in data solutions. These investments should recognize that a strong health care sector is a core pillar of the knowledge economy and as a subset, the innovation economy.
- The Province of Ontario must put in place a framework that advances the innovation economy of Ontario by linking Ontario’s digital health assets to the many innovation hubs in Ontario.
- The Province of Ontario should put in place a legal and policy framework that enables the province’s many innovators, entrepreneurs, innovation hubs and research institutes to further realize the potential of our digital health assets to advance knowledge through research, to improve patient outcomes, to reduce health care costs and grow jobs in Ontario, while protecting the health system’s core values and patient privacy.
- The Secretariat should work with partners – including the Information and Privacy Commissioner, innovation hubs, the Institute for Clinical Evaluative Sciences, Health Quality Ontario, and Ontario’s Chief Health Innovation Strategist – to grow the extent to which Ontarians benefit from privacy-sensitive analysis of health data, for example by enabling follow-up with patients whose health needs are not being met and by improving understanding of patterns of health, disease, and health care outcomes.
Appendix A – Expert individuals and groups engaged
- Ministry of Health and Long-Term Care (PDF)
- eHealth Ontario (PDF)
- Dr. Mohamed Alarakhia, Director, The Centre for Family Medicine Fht eHealth Centre of Excellence (PDF), Physician Lead, Waterloo Wellington Local Health Integration Network (LHIN) Enabling Technologies, Assistant Clinical Professor, McMaster University, and Adjunct Professor, University of Waterloo
- Matthew Anderson, President & CEO, William Osler Health System - letter (PDF), paper (PDF)
- Dr. Michael Apkon, President & CEO, Sick Kids Hospital (PDF)
- Michael Barrett, CEO, South West LHIN (PDF)
- Brian Beamish, Information and Privacy Commissioner of Ontario (PDF)
- Duane Bender, Director, Digital Health Applied Research at Mohawk College (PDF)
- Catherine Brown, CEO, Ontario Association of Community Care Access Centres (PDF)
- Dr. Ed Brown, Founder & CEO, Ontario Telemedicine Network (PDF)
- Donna Cripps, CEO, Hamilton Niagara Haldimand Brant LHIN (PDF)
- Anthony Dale, President & CEO, Ontario Hospital Association (PDF)
- Susan Fitzpatrick, CEO, Toronto Central LHIN (PDF)
- Murray Glendining, President & CEO, London Health Sciences Centre (PDF)
- Michael Green, President & CEO, Canada Health Infoway - briefing note (PDF), presentation (PDF)
- Dr. Doris Grinspun, CEO, Registered Nurses Association of Ontario (PDF)
- Dr. John Halamka (PDF), International Health Care Innovation Professor at Harvard Medical School and Chief Information Officer of the Beth Israel Deaconess Medical Center
- Angie Heydon, Chief Executive Director, Association of Family Health Teams of Ontario (PDF)
- Sarah Hutchison, CEO, Ontario MD (PDF)
- Dr. Jack Kitts, President & CEO, The Ottawa Hospital (PDF)
- Chantale LeClerc, CEO, Champlain LHIN Eastern Ontario-Ottawa Renfrew
- David MacDonald, Secretary, President & CEO, Hospital Diagnostic Imaging Repository Services (PDF)
- Dr. Barry McLellan, President & CEO, Sunnybrook Health Sciences Centre (PDF)
- Dr. Peter Pisters, President & CEO, University Health Network (PDF)
- Dr. Michael Schull, President & CEO, Institute for Clinical Evaluative Sciences (PDF)
- Dan Sheldon (PDF), Digital Strategy Lead for the UK Department of Health
- Dr. Michael Sherar, President & CEO, Cancer Care Ontario
- Graham Scott (PDF), Chair of the Board, Canada Health Infoway
- Dr. Joshua Tepper, President & CEO, Health Quality Ontario (PDF)
- Adrianna Tetley, CEO, Association of Ontario Health Centres (PDF)
- Ilse Treurnicht, CEO, MaRS Discovery District (PDF)
- Dr. Virginia M. Walley, President, Ontario Medical Association (PDF)
- Jennifer Zelmer (PDF), President, Azimuth Health Group and previous Executive Vice-President at Canada Health Infoway
Appendix B - Open letter to Ed Clark (PDF)
October 7, 2016
Further to our discussions, I am writing to seek your expert advice based on your experience in valuing public and private assets with respect to Ontario’s digital health strategy.
As you know, over the last eight years, Ontario’s health care system partners have worked steadily to establish a connected health information network with leadership from eHealth Ontario. eHealth was established in 2008 with a mandate to facilitate the establishment and maintenance of electronic health records for all of Ontario’s residents. While the agency has encountered some setbacks and challenges, significant progress toward this goal has been achieved. Nearly all residents of Ontario who have interacted with the health system now have health records that are electronic. Most family physicians in our province have electronic medical records in their practices. In addition, nearly all hospital-based diagnostic imaging is now digital and key lab results are now available through a provincial information system
These systems have generated significant value for Ontario. In its 2015-16 annual report, Canada Health Infoway – the federal/provincial body charged with overseeing the use of innovative digital health solutions to improve Canadians' health – estimated that since 2007, digital health systems have produced an estimated $16 billion in benefits nationally. It is acknowledged that Ontario’s share of the national benefits is substantial. In fact, a report prepared by CHI looking specifically at Ontario health technology accomplishments shows that the province is leading the country in several key areas.
Today, I am writing to you as the Premier’s Business Advisor and Chair of the Advisory Council on Government Assets to assess and validate the value these systems have created for Ontario and to recommend ways to take them to the next level. Specifically, I am asking you to consider advising the government on two key issues with support from experts in digital health, as appropriate. First, I would ask you to provide the government with a value assessment of Ontario’s digital health assets and all related intellectual property and infrastructure. Secondly, please provide us with recommendations related to how to maximize the value of these assets for Ontarians by improving how care is delivered, the patient experience in interacting with the health care system and, indirectly, through the economic value that is created for Ontario’s economy. To inform the valuation, I would ask that you engage an international expert in digital health, such as Dr. John Halamka. In addition, please seek advice from the Information and Privacy Commissioner’s Office of Ontario to ensure the protection of personal health information in all recommendations.
I believe there is growing opportunity in moving to a digital health care system. Consistent with the government’s Digital Government plan, as announced in the 2016 Budget, our focus is shifting from providers to patients. We already have the infrastructure in place to connect and equip physicians, hospitals and other health care providers. Now, we need to focus on patient and consumer-focused tools and services that enable direct access to health information and improved care, such as accessing an individual’s own health records, booking physician appointments online, keeping track of medicines, renewing prescriptions electronically, accessing services and advice remotely, and more. This is the direction that will serve emerging public and patient needs.
As the mandate of eHealth Ontario nears expiry at the end of December 2017, I feel now is the opportunity to renew our vision for digital health as part of our work to transform our health-care system into one that is truly patient-centred. Shortly, my ministry will be consulting with patients, health stakeholders and digital health experts about a new digital health strategy. But the full extent and value of our existing digital health assets must be fully understood if we are to move forward with a new vision.
I want to be absolutely clear that in the course of your work on digital health and your resulting recommendation(s), the protection of personal health information is paramount. Enormous energy, resources and intellectual effort have been dedicated to ensuring the integrity and privacy of people’s personal health information. The purpose of this work is to better understand the value of our digital assets to help guide, in combination with the advice of other experts, Ontario’s future digital health strategy.
I hope you will accept my request to lead this work, and would welcome your advice before the end of December 2016 so that we can assess this information in advance of the final year of the agency’s current mandate.
Signed,
Dr. Eric Hoskins
Minister of Health and Long-Term Care